Diabetic-Friendly
Meal Plan
Meals built on nutrition science to support steady blood sugar, long-term health and fit real life in the UAE.
100% risk-free, Pause, Skip or Cancel anytime.
4m+ meals delivered
Rated ⭐ 4.7 Google 1.4k+ reviews
Free delivery anywhere in UAE
Understanding diabetes beyond the medical talk
- Diabetes is when your body can’t use sugar the way it should. Instead of turning into energy, it stays in your blood, and that can later damage important organs.
- Normally, your body uses insulin to move sugar from your bloodstream into your cells, kind of like opening a door so energy can get in.
- But when there isn’t enough insulin or it doesn’t work the way it should, that sugar just hangs around in your blood.
- Over time, consistently high blood sugar can damage the heart, kidneys, eyes, nerves, and feet.
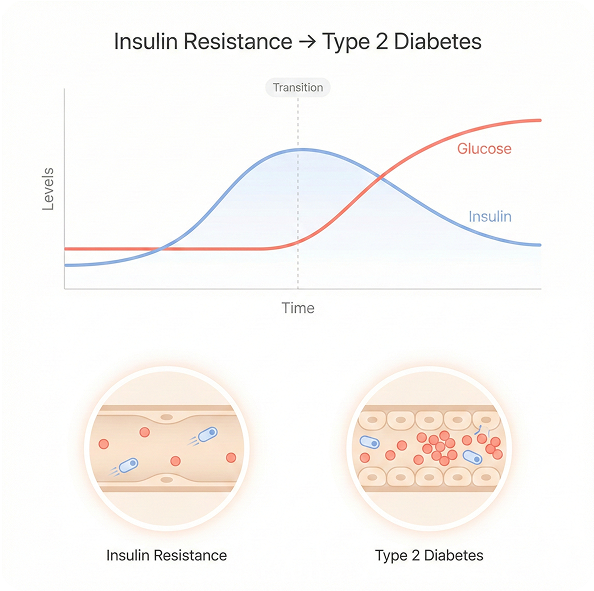
This is a simplified illustration. Individual insulin and
glucose responses may vary.
glucose responses may vary.

Did you know?
According to the World Health Organization, diabetes is one of the fastest-growing chronic conditions worldwide, largely driven by diet, lifestyle, physical inactivity, weight patterns and genetics.
Types of diabetes and what
actually changes on your plate
Hot tip: - The American Diabetes Association confirms that nutrition therapy is a
first-line treatment for Type 2 diabetes and pre-diabetes.
Why is managing diabetes
more than just cutting sugar?
Many people think managing diabetes means avoiding sugar alone. In reality, total carbohydrate intake, portion sizes, food quality, and food combinations matter far more.
What raises blood sugar fastest
- Refined carbohydrates (white bread, pastries, sugary drinks)
- Large portions eaten on their own
What keeps blood sugar steady
- Pairing carbs with protein and healthy fats
- Eating fibre-rich foods
- Keeping regular meal timing
Ready to feel in
control again?
Eating for diabetes doesn’t mean restriction, it means structure, balance, and consistency that works in real life. Research from the Harvard School of Public Health shows that balanced meals slow glucose absorption and reduce post-meal blood sugar spikes.
Everyday benefits of a
diabetic-friendly meal plan
Glycemic Index vs.
Glycemic Load:
What really matters for diabetes
“Simple” or “complex” doesn’t always explain what they actually do to your blood sugar.
That’s where glycemic index (GI) and glycemic load (GL) are more useful.
The Glycemic Index is about speed.
It tells you how quickly a food raises blood sugar. Foods like white bread or sugary cereals raise it fast, while foods like oats or lentils raise it more slowly.
The Glycemic Load looks at the real-life impact.
It considers both how fast blood sugar rises and how much it rises, based on portion size. That’s why it matters more day to day.
A couple of things to keep in mind:
- A food with a high GI can still be okay if the portion is small.
- A food with a low GI can still cause a spike if you eat a lot of it.
In short: Aim for foods with a low or medium glycemic load most of the time, and keep high-glycemic-load foods as occasional treats. It’s an easier way to keep blood sugar steadier without overthinking every bite.
Foods to rely on
- Non-starchy vegetables: spinach, broccoli, peppers
- Lean proteins: fish, chicken, eggs, tofu, lentils
- Whole grains: oats, quinoa, brown rice (portioned)
- Healthy fats: olive oil, nuts, seeds, avocado
- Fruits (portioned): berries, apples, citrus
Foods to limit
- Sugary drinks and juices
- White bread, pastries
- Large portions of rice or pasta eaten alone
- Deep-fried foods
Types of diabetes and what actually changes on your plate
The Centers for Disease Control and Prevention emphasises moderation and balance, not restriction, for long-term diabetes management.

Eating out & takeout:
how
to stay in control
Takeout is built for flavour and big portions, not blood sugar control. Hidden sugars, refined carbs, and extra oils can push sugar levels higher than you realise and slow progress over time.
Delicut helps by taking the guesswork out, with portion-controlled, balanced meals designed to keep blood sugar steady and fit real UAE lifestyles.
Sample Diabetic-
Friendly Meal Plan
7 day daily structure (balanced)
100-120g
Daily Protein
1400-1600
Daily Calorie
4-5
Meals/day
Meal
Description
Breakfast
Vegetable omelette + whole-grain toast
Lunch
Baked fish, sautéed greens, small portion brown rice
Snack
Greek yogurt with nuts
Dinner
Grilled chicken, quinoa, roasted vegetables
Diabetes Macro Guidelines
Note: These macro ranges are practical nutrition planning guidelines, not medical prescriptions. Individual needs vary based on age, sex, activity level, medications, and health conditions. People with diabetes should personalise intake with a qualified healthcare professional
Goal
Protein
(g/kg)
Carbs
(g/kg)
Fats
(g/kg)
General diabetes support
1.2-1.4
2.0-3.0
0.8-1.0
Blood sugar control & weight management
1.4-1.8
1.8-2.5
0.8-1.0
Insulin sensitivity & metabolic health
1.3-1.6
2.0-2.8
0.9-1.1
Active lifestyle / training (diabetes-friendly)
1.6 – 2.0
2.5-3.5
0.9-1.1
40+ years (metabolic & muscle support)
1.4-1.8
2.0 – 3.0
0.9-1.1
Smart lifestyle changes for
managing diabetes every day
Eat balanced, regular meals
Focus on whole foods, controlled portions, and consistent meal timings to keep blood sugar steady.
Stay physically active
Daily movement like walking or light strength training improves insulin sensitivity and energy levels.
Prioritize quality sleep
Getting 7–9 hours of sleep helps regulate hormones that directly affect blood sugar.
Manage stress effectively
Reducing stress through mindfulness or relaxation prevents stress-related glucose spikes.
Monitor blood sugar consistently
Regular checks help you understand patterns and make timely adjustments.
Avoid smoking & limit alcohol
Cutting back protects your heart and prevents sudden blood sugar fluctuations.
Common
diabetes myths
& concerns,
clarified
If I'm on medication, does the food still matter?
Medication helps, but food choices still shape daily blood sugar levels. Nutrition and medication work best when they support each other.
Are fruits bad for diabetes?
Fruit isn't the problem - portions are. Whole fruits with fibre (like berries, apples, citrus) can fit into a diabetes-friendly diet when eaten mindfully.
Is Diabetes only caused by sugar?
Diabetes is influenced by overall diet, weight, activity level, genetics, and insulin response - not sugar alone.
Is diabetes reversible?
Yes, in some cases, it is reversible.
- Prediabetes is often reversible with lifestyle changes.
- Early Type 2 diabetes remission is possible for some people.
- Type 1 diabetes is not reversible, but very manageable.
Expert
nutrition advice
Get support from certified professionals who actually get how Middle Eastern diets and lifestyles work.
They bring global know-how with local understanding, so the advice feels relevant, realistic, and built for you.

Saja Davood
Registered Nutritionist with a degree in Food Nutrition and Dietetics
Clinical expertise
Specialises in developing evidence-based nutrition plans tailored to individual health conditions and dietary needs.Includes managing a wide range of conditions such as diabetes, hypertension, cardiovascular disease, obesity, gastrointestinal disorders, and PCOS.
Provides medical nutrition therapy (MNT) to support patients in preventing and managing chronic diseases through customized dietary interventions and lifestyle modifications.
Experience of + 5 years
Designation Nutritionist
Got questions?
We're here to help
What is the best meal plan for diabetes?
There isn't one "perfect" plan. The best diabetes meal plan is one that keeps blood sugar steady by balancing carbs, protein, fats, and fibre, while fitting your lifestyle so you can stick to it long term.
Do people with diabetes have to stop eating carbs?
No. Carbs don't need to be eliminated, they need to be managed. Choosing better-quality carbs, watching portions, and pairing them with protein and fibre makes a big difference.
How many meals should a person with diabetes eat per day?
Most people do well with 3 main meals and 1–2 small snacks. Regular eating helps prevent big blood sugar highs and lows, especially if you're on medication.
Is rice completely off-limits for diabetes?
No. Rice can still fit into a diabetes-friendly diet, it's about portion size, type, and pairing. Smaller portions, eaten with protein and vegetables, are easier on blood sugar.
Is a high-protein diet safe for diabetes?
Yes, for most people. Protein helps slow digestion, reduce cravings, and stabilise blood sugar. If you have existing kidney issues, it's best to follow a plan guided by a professional.
View all FAQs
4M+ meals delivered / 125K+ happy customers /4M+ meals delivered / 125K+ happy customers /4M+ meals delivered / 125K+ happy customers /4M+ meals delivered / 125K+ happy customers /